According to data from the World Health Organisation, about 15% of couples of childbearing age experience difficulties in conceiving naturally, with an increasing trend linked to social, environmental and health factors.
The use of medically assisted procreation techniques (PMA) has grown exponentially in recent decades, but the structural limits of these treatments remain evident.
The use of medically assisted procreation (MAP) techniques has grown exponentially in recent decades, but the structural limitations of these treatments remain evident. The average success rate per cycle of in vitro fertilisation (IVF) is still between 25% and 30%, despite technological advances and accumulated clinical experience. Each unsuccessful attempt entails not only significant economic costs, but also a significant emotional impact on patients.
One of the main obstacles lies in the inherent complexity of treatment pathways: each patient represents a unique case, characterised by biological, genetic, clinical and behavioural variables that are difficult to standardise. The management of this — heterogeneous and constantly updated data — requires tools capable of processing complex information and returning personalised indications.
Predictive algorithms applied to fertility are able to analyse large volumes of clinical data, detect hidden patterns and suggest optimised therapeutic strategies. First concrete applications in assisted reproduction centres have already shown significant results: AI-based systems have achieved a predictive accuracy of up to 73-75% in the selection of embryos most likely to be implanted, and customised protocols supported by AI models have made it possible to reduce the risk of complications related to ovarian hyperstimulation by up to 30%.
The contribution of AI to fertility research is now available in the UK.
The contribution of AI is not only limited to improving clinical performance, but also has a profound effect on the quality of care and personalisation of treatments, opening up a new paradigm of reproductive medicine based on data, precision and innovation.
Artificial Intelligence as Clinical Decision Support System (CDSS) in Infertility Pathways
Infertility is a condition that requires extreme precision in clinical management. Each medically assisted procreation treatment is characterised by many variables: ovarian reserve, drug response, oocyte and embryo quality, genetic and environmental factors. Artificial intelligence fits into this context as an operational tool for precision medicine, intervening at the most delicate decision-making moments.
Clinical Decision Support Systems (CDSS) based on AI do not merely automate procedures, but represent engines for personalising therapies. Using predictive models and machine learning, these systems rapidly process large amounts of individual clinical data and return personalised suggestions for:
- dosing of drugs in ovarian stimulation;
- the choice of hormone support protocols;
- the identification of the optimal time for oocyte pick-up;
- the selection of embryos with the greatest evolutionary potential;
A distinctive feature of these tools is their ability to significantly reduce the subjective component of certain phases of reproductive medicine, traditionally entrusted to individual experience and intuition. Advanced image analysis systems, for example, allow the morphological and dynamic characteristics of embryos to be analysed objectively and standardised, thus helping to limit variations in judgement between operators and clinical centres.
This is flanked by the evolution of Large Language Models (LLM), which allow CDSS to read and understand even complex clinical documentation, medical histories, electronic medical records and up-to-date scientific studies. Their implementation in fertilisation centres makes it possible to integrate not only structured data (numerical or laboratory), but also narrative and textual data, completing the global view of the patient.
The result of this transformation is twofold: on the one hand, the physician is supported in making more informed and data-driven clinical choices, and on the other hand, the patient receives a more targeted treatment, potentially more effective and with fewer side effects.
The implementation of the Fertilisation Centre's data allows the integration of not only structured data (numerical or laboratory), but also narrative and textual data, thus completing the patient's global view.
Artificial intelligence, in this scenario, is configured not as an alternative to the doctor, but as an extension of his or her decision-making capabilities, amplifying his or her competences thanks to computational power and predictive analysis.
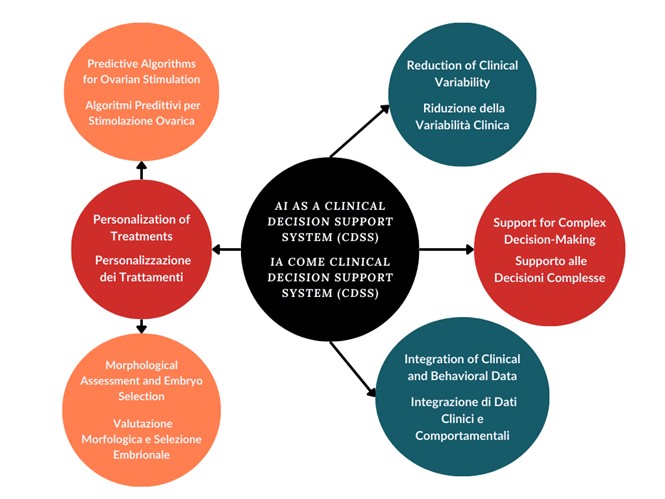
Conceptual map of the main applications of Artificial Intelligence as a clinical decision support system (CDSS) in infertility pathways.
Data Integration: An Organisational and Management Priority
Without a complete and accurate information base, even the best predictive models are ineffective or even misleading.
The first major qualitative leap required of reproductive medicine centres concerns the ability to collect, organise and integrate complex clinical data in a systematic way. Individual medical expertise, although fundamental, is no longer sufficient in the face of the increasing complexity of patients' reproductive profiles.
These processes generate a great deal of data, which is not always available.
These processes generate enormous amounts of information: hormonal examinations, ultrasound characteristics, ovarian stimulation progress, genetic parameters, embryonic quality, past medical history. To these are added behavioural and environmental data — such as lifestyle, stress level, sleep quality or diet — which may significantly influence the response to treatments.
All these data, to be useful, must be:
- collected in a homogenous and standardised manner;
- archived in interoperable and secure systems;
- easily accessible for processing and analysis;
&This is where a decisive part of the future quality of infertility treatment is at stake. The centres that know how to build integrated digital ecosystems, capable of collecting structured and unstructured data throughout the treatment pathway, will be the ones able to truly exploit the potential of artificial intelligence.
Multidimensional data analysis is therefore not a technological 'plus', but a prerequisite for personalised, predictive and precision reproductive medicine.
In addition to its strictly clinical purpose, this advanced information management capability also produces clear operational benefits: reduction of human errors, greater traceability of treatment pathways, possibility of auditing and verification of results, and improvement of decision-making and communication processes within multidisciplinary teams.
In the end, there is no effective artificial intelligence without a solid and widespread data culture. And in reproductive medicine — perhaps more so than in other fields — data is not just technical information, but the key to interpreting the biological and human complexity of each patient.
Biases and Ethical Risks in Artificial Intelligence Models Applied to Fertility
The real effectiveness of these technologies and their clinical acceptability depend on the ability to responsibly manage the ethical risks and structural limitations that accompany these tools.
Among the main critical elements is the problem of algorithmic bias: artificial intelligence models are not independently unbiased. The quality of their predictions depends on the quality of the data used to train them. If these data do not reflect the real diversity of populations, the results produced risk being biased or unreliable for all patients.
This phenomenon assumes particular relevance in medically assisted reproduction pathways, where a large part of the available dataset comes from patients belonging to well-defined geographical and genetic populations — mostly of Caucasian origin and from European or North American clinical settings. The indiscriminate application of these models to patients of other ethnicities or with different biological characteristics could lead to less accurate predictions, irrelevant therapeutic suggestions or even clinical errors.
In addition to the risk of bias, there are other relevant ethical issues related to the use of AI in reproductive medicine. The transparency of algorithms — often referred to as the 'black box' — is a crucial issue: many of the predictive systems currently in use do not allow for a full understanding of how the recommendations provided to clinicians are processed. This opacity can reduce patient confidence and complicate medical-legal liability in the event of disputes.
The management of reproductive data, moreover, requires particularly high security standards. The health information processed in fertility treatments is among the most sensitive of all, because it involves aspects related to the intimate, genetic and family spheres of patients. The protection of these data and their proper management is an unavoidable ethical and regulatory obligation.
At the regulatory level, the European Union has already embarked on specific regulation on the use of AI in healthcare, with the aim of defining common standards of security, transparency and respect for patients' rights.
Towards Data-Driven Reproductive Medicine: Conclusions
Today, at least 11 Clinical Decision Support System (CDSS) algorithms applicable to clinical and laboratory management of medically assisted reproduction pathways have already been identified. These tools, developed to support decisions in areas such as ovarian stimulation, embryo evaluation and drug dosage management, represent the state of the art of artificial intelligence applications in infertility treatments.
However, available data indicate that the widespread and safe adoption of these models will still require important steps forward. In particular, the systematic review of the main international studies points to the presence of very heterogeneous validation methods, with non-standardised verification protocols and little comparability between them.
The most important point of arrival is the need for a more comprehensive validation process.
The most mature point of arrival of this transformation is not only technological, but first and foremost organisational and cultural. Artificial intelligence will only be able to express its full potential in reproductive medicine when digital ecosystems are built that are truly capable of collecting, managing, integrating and exploiting complex data in a systematic and secure manner.
The most mature point of arrival of this transformation is not only technological, but first and foremost organisational and cultural.
Bibliographic References
Artificial Intelligence, Clinical Decision Support Algorithms, Mathematical Models, Calculators Applications in Infertility: Systematic Review and Hands-On Digital Applications
Carlo Bulletti, MD; Jason M. Franasiak, MD; Andrea Busnelli, MD; Romualdo Sciorio, BSc, Msc; Marco Berrettini, PhD; Lusine Aghajanova, MD, PhD; Francesco M. Bulletti, MD; and Baris Ata, MD
Transforming Health Care With Artificial Intelligence: Redefining Medical Documentation
Archana Reddy Bongurala, MD; Dhaval Save, MD; Ankit Virmani, MSc; and Rahul Kashyap, MBBS
Transforming Large Language Models into Superior Clinical Decision Support Tools by Embedding Clinical Practice Guidelines
Yanshan Wang, PhDa,b,c,d; Xiaoxi Yao, PhD, MPHe,f; and Xizhi Wua• Car J, Sheikh A, Wicks P, Williams MS.
https://doi.org/10.1016/j.mcpdig.2024.05.018
How are Machine Learning and Artificial Intelligence Used in Digital Behavior Change Interventions? A Scoping Review
Amy Bucher, PhD; E. Susanne Blazek, PhD; and Christopher T. Symons, PhD